
Oral Cancer Exams and Biopsies for the GP
What if there was a very simple exam that you could do as part of every routine dental exam that could potentially save a patient’s life? Well, there is: an oral cancer screening. In 2022, approximately 54,000 Americans were diagnosed with oral cancer, and about 11,000 people lost their lives to this disease. As a general practitioner, you are on the front line of detection for this potentially deadly disease.
Dr. Robert Convissar, a general practitioner with over 40
years of clinical experience who maintains a private practice in New York City
and lectures worldwide on laser surgery and biopsy techniques, believes that
both oral cancer exams and simple biopsies should be within the general
practitioner’s purview.
How to do an oral cancer exam
A basic oral cancer exam is quite simple. “All you need,” Dr. Convissar explains, “is a regular dental mirror, a piece of gauze and your eyeballs, that’s it. It’s just a matter of using your fingers to palpate everything. Take a look, make sure everything looks pink and healthy. Make sure there are no lumps or bumps. Make sure that everything looks relatively normal bilaterally, that there’s nothing unusual.”
“The number one site for malignancies in the oral cavity is the lateral board of the tongue,” he adds. “So you just take a piece of gauze, wrap it around the tongue, pull the tongue out as far as you can, move the tongue to the left, move the tongue to the right, check both lateral borders, move it up, check down to the root of the tongue, and that’s basically it.”
If you want, you can also add some additional tools to your arsenal in order to make the oral cancer exam even more thorough:
· Pharyngeal
mirror – This is a dental mirror with a very long handle that
enables you to look all the way down to the root of the tongue, where
malignancies can also occur. To avoid making the patient gag, be sure to hold
the pharyngeal mirror halfway between the tongue and the palate – not on the
tongue or the palate.
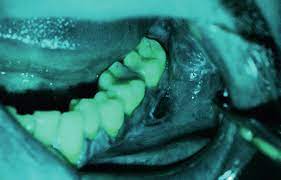
· GOCCLES®
oral cancer screening glasses – These are special glasses from Pierrel
that filter out specific wavelengths. Put on the glasses and then use your
curing light to illuminate the inside of your patient’s mouth. The GOCCLES®
will then enable you to differentiate between fast-growing and slow-growing
tissue.
“Cancer malignancies tend to have a higher mitotic activity than normal tissue,”
Dr. Convissar states. “So when you put on the GOCCLES® and use your
curing light, you can tell there’s a difference in the fluorescence of the
tissue. This doesn’t mean cancer; it just means it’s something that you must
investigate further. And a biopsy would be a great way to investigate.”
Note that there is an ADA diagnostic code that enables you to bill for this
type of exam with many (but not all) insurance providers.
[blogad]
What to do if you see something suspicious
The good news about doing oral cancer screenings is that the
top 24 or so types of lesions that general practitioners see – such as lichen
planus, mucous striations, ulcerations and abscesses – are most likely benign. To
help you make the determination, Dr. Convissar has developed a pneumonic
device, “FIGRUB.” Each letter of this made-up word stands for one of the six
qualities that can determine if a lesion is most likely benign or malignant.
· Fixed: If a
lesion is fixed to the underlying tissue and not freely movable, it could be
malignant. If it’s freely movable, it’s most likely benign.
· Indurated: If it’s
indurated, it is probably malignant. If it’s not indurated, if it’s nice and
soft, it’s probably benign.
· Growth: If it
has been growing very slowly, it is most likely benign. If it has grown
quickly, such as if it wasn’t there a week ago and now it’s there and getting
larger, it could be malignant.
· Red or
White, or Red and White: If a lesion looks red or white, or it
looks both red and white, it could be malignant. If it’s neither red nor white,
it could be benign.
· Ulcerated: If
the surface epithelium or the surface mucosa of the lesion is ulcerated, that
could mean that it is malignant. If it’s not ulcerated, it could be benign.
· Bleeds: If it bleeds easily, without you poking around at it, it could be malignant. If it doesn’t bleed easily, it could be benign.
If you see three of these characteristics, there’s a good
probability that it’s malignant – provided you also temper your judgement with
a little bit of common sense as well as knowledge of what is normal anatomy. “If
I’m looking at somebody’s palate,” Dr. Convissar points out, “and they have a
lesion that’s fixed and indurated and ulcerated, well that’s three out of the
six qualifications. But if it’s on the palate, it may be nothing more than a palatal
torus with a pizza burn on it.”
Should you do a biopsy?
Once you complete this evaluation, if the situation is still suspicious you need to decide if it’s in an area where you feel comfortable performing a biopsy. For this, Dr. Convissar recommends that you consider:
· Location
–
If it’s on the soft palate or the junction of the soft and hard palate, this
may be difficult for a general practitioner. But if it’s on the buccal mucosa,
this is much easier.
· Hemostasis
–
Is it in the midline of the palate where there are not a lot of blood vessels? Or
is it closer to the teeth, where you may have the posterior superior alveolar
arterials to worry about?
· Training – “If you are trained in biopsy technique,” Dr. Convissar says, “it’s really a very, very simple thing to do. Training, training, training are the three important criteria for deciding if you want to biopsy it and if you feel confident to biopsy it.”
In terms of equipment, all you need is some sort of cutting
device (laser, 15 blade, punch, cryosurgery, electro-surgery) and a suture set
up to suture the lesion if it needs suturing, and that’s basically it.
Everything else will be in the biopsy kit from the oral pathology lab.
Conclusion
Oral cancer screenings save lives. As a general practitioner
you should be talking to your patients about this, and making it an important
part of your routine dental exams.























